We all know how important it is to brush our teeth every day—but have you ever wondered whether it’s better to use an electric toothbrush or a regular manual one?
Both electric and manual toothbrushes can clean your teeth effectively, but they have different features, advantages, and costs. Let’s explore the differences and help you decide which one might be the better fit for your dental routine.
Manual Toothbrush: The Traditional Choice
The manual toothbrush has been around for over a century, and for good reason—it works.
Advantages of Manual Toothbrushes:
- Affordable: You can find a decent manual toothbrush almost anywhere, and they usually cost just a few dollars.
- Portable and Simple: No batteries, no chargers. Perfect for travel or emergencies.
- Variety: Available in different bristle strengths, head sizes, and handle designs.
Downsides:
- Technique Matters: How well it works depends on your brushing technique. It’s easy to miss spots or apply too much pressure.
- No Timer: Without a built-in timer, it’s up to you to make sure you’re brushing for the recommended 2 minutes.
Electric Toothbrush: The Smart Option
Electric toothbrushes have become increasingly popular, and many dentists recommend them for their extra cleaning power.
Advantages of Electric Toothbrushes:
- More Effective Cleaning: Many studies show electric brushes remove more plaque than manual ones, especially oscillating-rotating models.
- Built-in Timers and Modes: Most come with timers and pressure sensors to improve your brushing technique.
- Great for Kids and Those With Limited Mobility: Ideal for people who struggle with manual brushing or lack coordination.
Downsides:
- More Expensive: Costs can range from $20 to over $200, plus replacement brush heads.
- Needs Power: Requires charging or battery replacements.
- Not As Travel-Friendly: Bulkier and requires extra space in your bag.
What Do Dentists Say?
Most dental professionals agree on this: It’s not just the brush—it’s how you use it.
You can have great oral hygiene with either type of toothbrush if you brush twice a day for two minutes, use fluoride toothpaste, and floss daily.
However, for people who:
- Tend to brush too hard
- Have trouble reaching all areas of their mouth
- Need extra help maintaining good habits
→ An electric toothbrush may offer better results.
Final Verdict: Which One Is Better?
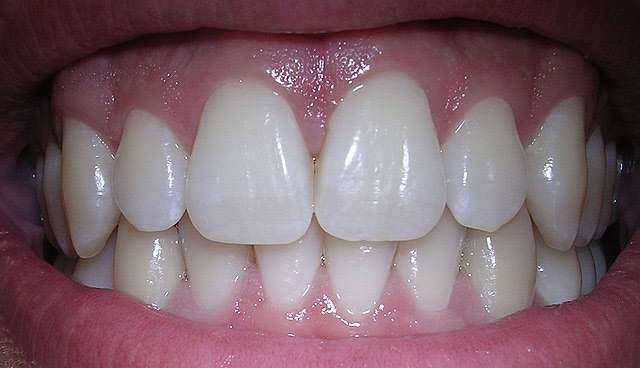
If your teeth look clean like this with your regular brushing
Then you can continue using your manual tooth brush optimally
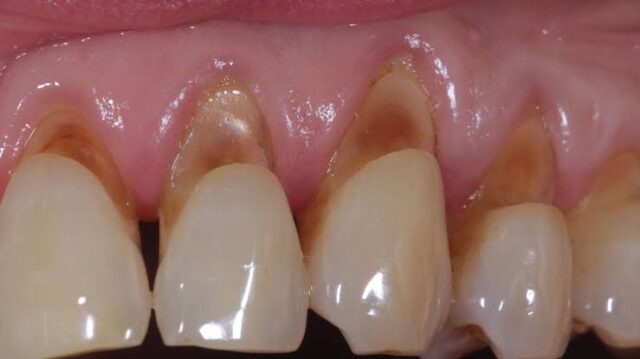
If you are suffering from tooth wear due to aggressive brushing electric tooth brush should be your choice of tool
At the end of the day, the best toothbrush is the one you’ll actually use—correctly and consistently.
Pro Tip: No matter which type you choose, replace your toothbrush (or brush head) every 3–4 months or sooner if the bristles are frayed.